Pulmonary Embolism: What is it, Symptoms, Diagnosis and Treatment
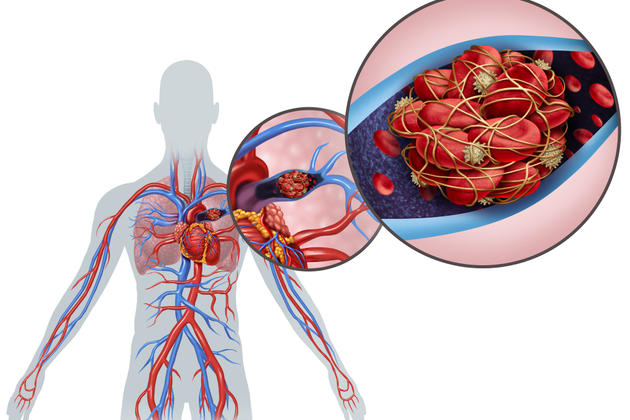
Pulmonary embolism, also known as pulmonary embolism, refers to blockage in the lung vessels due to various reasons. It usually occurs when a clot in the legs or elsewhere in the body travels through the circulation and blocks the lung artery. This condition disrupts the blood circulation in the lungs, causing problems in carrying oxygen to the cells and can cause significant respiratory problems.

What is Pulmonary Embolism?
Pulmonary embolism is the blockage of the lung arteries with a clot or other material. Pulmonary embolism usually occurs when a clot that forms in another part of the body (most often from deep venous thrombosis in the legs) travels through the bloodstream to the lungs. This blockage causes the lung arteries to narrow or become blocked, preventing adequate blood from reaching the lung tissue. Pulmonary embolism can affect the lungs’ oxygen exchange and lead to serious breathing problems. It can also disrupt the normal function of the lungs due to clots in the lung tissue and cause problems in the circulatory system between the heart and lungs.
What are the Symptoms of Pulmonary Embolism?
Symptoms and severity of pulmonary embolism may vary depending on the size and number of clots and the patient’s general health condition. The main symptoms of pulmonary embolism are:
- Sudden onset of severe chest pain
- Shortness of breath (especially increasing with exertion)
- rapid breathing
- Palpitations or fast heartbeat
- Cough (may contain blood and sputum)
- Weakness and dizziness
What Causes Pulmonary Embolism?
Pulmonary embolism usually occurs as a result of a combination of factors such as:
- Deep Venous Thrombosis (DVT): DVT is a condition in which clots form in the deep veins, usually in the legs. These clots can reach the lungs through the bloodstream and cause a pulmonary embolism.
- Immobility: Being inactive for long periods of time, such as being bedridden for long periods of time, long plane rides or car rides, can lead to slow blood circulation and clot formation.
- Surgical Procedures: During or after surgical procedures, keeping patients bedridden or restricting their movements may contribute to clot formation.
- Trauma and Fractures: Clot formation is more likely in areas where the vessels are damaged as a result of serious injuries, fractures or trauma.
- Cancer: Cancer can cause the release of certain substances that can affect blood clotting, thus making it easier for clots to form.
- Pregnancy: Changes in hormone levels during pregnancy can cause blood to clot more easily and increase the risk of pulmonary embolism during pregnancy.
- Heart Failure: Heart failure causes the heart to be unable to pump blood effectively and can lead to blood slowing down in the vessels and clot formation.
How is Pulmonary Embolism Diagnosed?
Diagnosis of pulmonary embolism (PE) is made through a combination of symptoms, medical history, and various tests. Diagnosing PE is one of the medical emergencies and it is important to do it quickly. Some common methods used to diagnose PE include:
- Physical Examination: The doctor obtains information about the patient’s symptoms and performs a physical examination. He listens to lung and heart sounds and evaluates the symptoms to pay attention to during the examination.
- Anamnesis (Medical History): Anamnesis is taken by taking into consideration factors such as the patient’s previous health condition, past clotting problems, immobility, surgical history, and pregnancy history.
- Blood Tests: A blood test called D-dimer can indicate clot formation in the body. However, D-dimer testing alone is not sufficient to make a definitive diagnosis of PE and additional tests are needed.
- Display Methods:
- a. Chest X-ray: There may be signs of clot-related changes in the lung, but it is not sufficient to diagnose PE.
- b. Spiral Computed Tomography (CT): It is the most commonly used imaging method for diagnosing PE. It can detect clots and blockages in the pulmonary arteries.
- c. Ventilation-Perfusion Scintigraphy (VQ Scintigraphy): Evaluates the distribution of air and blood flow in the lungs and helps evaluate the possibility of PE.
- D. Pulmonary Angiography: It is the method used for the most definitive diagnosis of PE. Detailed images of the lung arteries are taken by injecting contrast material through a catheter.
What are the Treatment Methods for Pulmonary Embolism?
Treatment for pulmonary embolism (PE) aims to dissolve the clot, prevent existing clots from growing, and prevent new clots from forming. The treatment plan is determined by the severity of PE, the patient’s general health and other medical conditions. Pulmonary embolism treatment methods include:
- Anticoagulants (Blood Thinners): Anticoagulant drugs help prevent clot formation by reducing the blood’s ability to clot. Injectable medications, such as heparin and low molecular weight heparin, or oral medications, such as warfarin, may be used. Heparin is a fast-acting medication and is usually started while hospitalized. Warfarin is used for long-term treatment and requires regular blood tests.
- Thrombolytic (Fibrinolytic) Treatment: If PE is severe or life-threatening, doctors may use thrombolytic medications. These medications help dissolve clots. Thrombolytic therapy is usually administered intravenously and is usually monitored as an inpatient because it carries a risk of bleeding.
- Surgical Embolectomy: Rarely, emergency surgery may be required to treat PE. In this case, a surgical embolectomy may be performed to physically remove large clots in the pulmonary artery.
- Filter Insertion: In some cases, a device called a vena cava filter may be inserted to prevent large clots that have moved away from the patient’s body from reaching the lungs.
- Supportive Treatment: If the patient needs respiratory support and oxygen support, supportive treatments are provided.
What Should Nutrition Be Like in Pulmonary Embolism?
For patients who have suffered a pulmonary embolism (PE), a healthy eating plan can help support healing and keep the body functioning healthily. Nutrition is important for PE treatment and overall health. Here are nutritional recommendations to consider for patients experiencing PE:
- Diet with Low Atherosclerotic Potential: Because PE is caused by atherosclerosis, it is important to limit or avoid foods rich in salt, saturated fats, trans fats, and cholesterol. These are usually processed foods, fatty meats, processed snacks and fast food.
- Adequate Fluid Intake: Drinking plenty of water can help regulate blood circulation and prevent blood clots. Water keeps the body hydrated and reduces blood clotting. However, it is also important to try to prevent water retention by keeping your salt intake under control.
- Low-Dose Aspirin: For some patients, doctors may prescribe low-dose aspirin. Aspirin may help reduce blood clotting, but should only be used with your doctor’s recommendation because it may have side effects or interactions with other medical conditions.
- Healthy Fats: It may be beneficial to add foods that contain healthy fats, omega-3 fatty acids, such as fish, avocado, olive oil and nuts to your diet. Omega-3 fatty acids may help protect blood vessels and heart health.
- Fiber Foods: Fibrous foods, such as fresh fruits, vegetables, whole grains and legumes, help regulate cholesterol levels and improve digestive health.
- Vitamin D and Vitamin K: Vitamin D increases calcium absorption, while vitamin K contributes to blood clotting. Therefore, while you get your vitamin D intake from sunlight or supplements, it’s important to keep your vitamin K intake balanced as well.
- Supplements: During treatment, you may need to take vitamin and mineral supplements recommended by your doctor.
What Should Not Be Consumed in Pulmonary Embolism?
The nutrition plan for patients with pulmonary embolism should be designed taking into account medical treatment and general health status. It is important not to consume or limit the following foods and drinks during PE treatment:
- Foods Containing High Salt: High salt intake can lead to water retention in the body and increased blood pressure. This may negatively affect blood vessels and heart health. Salty snacks, processed foods, canned goods and ready-made sauces may contain high amounts of salt.
- Saturated and Trans Fats: Saturated fats and trans fats can raise cholesterol levels and increase the risk of atherosclerosis. These types of fats are found in red meat, full-fat milk and dairy products, processed snacks, and fast foods. Therefore, it is important to limit sources of saturated fat, such as butter and margarine.
- Highly Sugary Foods and Drinks: Excessive sugar consumption increases insulin levels and can cause blood sugar fluctuations. It is important to limit consumption of sugary drinks, snacks and desserts with added sugar.
- Foods Containing Excessive Cholesterol: It is important to limit foods containing cholesterol. These are often found in animal-derived products such as red meat, egg yolks and processed snacks.
- Foods High in Vitamin K: If anticoagulant medications are used during treatment, it is important to limit or balance the consumption of foods containing vitamin K, which affects the blood’s ability to clot. These are often found in green leafy vegetables (such as spinach, broccoli, kale) and some vegetable oils.
What is Embolism Stocking?
Embolism stocking, also known as compression stocking, is a special medical stocking used to reduce the risk of deep vein thrombosis (DVT) or prevent the formation of pulmonary embolism (PE). Embolism stockings are designed to ensure better blood circulation in the legs and prevent blood from pooling. The compression of the muscles and veins in the legs by the socks helps reduce blood accumulation in the legs and clot formation by increasing venous return (the return of blood to the heart). Embolism stockings are generally used for long-term bed rest, surgical operations, or in people at risk of DVT, especially during long-term travel. It can also be used in people with swelling in the legs or circulation problems.



… [Trackback]
[…] Informations on that Topic: pressug.com/pulmonary-embolism-what-is-it-symptoms-diagnosis-and-treatment-2/ […]