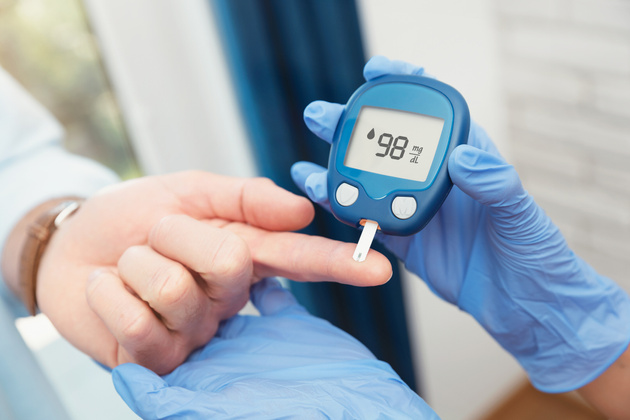
What is Diabetes? What are the symptoms of diabetes?
Most people know diabetes as “diabetes mellitus”. However, this is only one side of the matter. Diabetes mellitus, which we simply call diabetes, is a chronic disease caused by high levels of glucose (sugar) in the blood circulation system.
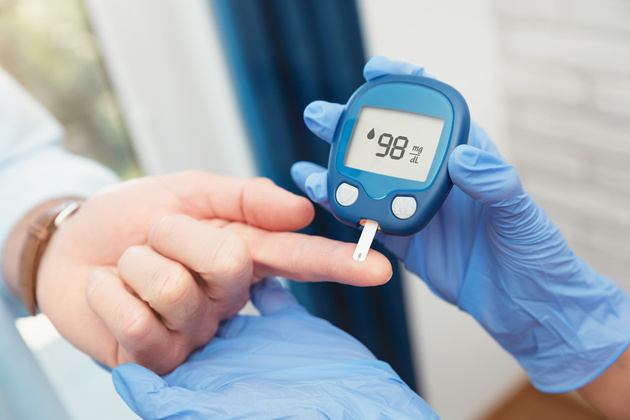
What is diabetes?
Most people know diabetes as “diabetes mellitus”. However, this is only one side of the matter. Diabetes mellitus, which we simply call diabetes, is a chronic disease caused by high levels of glucose (sugar) in the blood circulation system. The word “diabetes” is a combination of the Greek words “siphon” (a tube bent in half through which liquid flows) and the Latin “mellitus” meaning “sweet as honey”. This name describes the disease literally: Constant thirst and frequent urination are symptoms specific to diabetes. These symptoms result from the pancreas producing insufficient insulin or the resistance of body tissues to the action of insulin—or a combination of the two. To understand what this means, it is necessary to know where the glucose in our body comes from, what it is used for, and how it is regulated by insulin.
What are the symptoms of diabetes?
The most common early symptom of diabetes is increased thirst and frequent urination. These initial symptoms are often linked to hyperglycemia, the scientific name for high blood glucose levels.
Common symptoms of diabetes include:
- increased hunger
- increased thirst
- weight loss
- frequent urination
- blurred vision
- Overstrain
- wounds that do not heal
In addition, men may experience symptoms such as decreased sexual desire and erectile dysfunction (ED), while women may experience symptoms such as urinary tract infections, yeast infection and dry, itchy skin lesions.
What are the types of diabetes?
Although there are several types of diabetes, the two most common types are:
- Type 1 Diabetes
- Type 2 Diabetes
What is type 1 diabetes?
It usually starts before the age of 30 and occurs suddenly in people of normal weight. In this type (formerly known as insulin-dependent diabetes), the immune system attacks and destroys the beta cells of the pancreas, leaving the pancreas unable to produce enough insulin. Since it usually starts in childhood, Type 1 diabetes is also called early-onset diabetes. It can also occur in adults, but is much less common. Type 1 diabetes is a serious disease that cannot be cured simply by losing weight or paying attention to what you eat. Patients with type 1 diabetes must take insulin injections several times each day to prevent blood sugar from rising to fatal levels and avoid long-term complications.
What are the symptoms of type 1 diabetes?
The initial symptoms of type 1 diabetes often appear suddenly, sometimes quite frighteningly. When insulin production decreases, glucose accumulates in the circulatory system instead of being transported to body cells that need it for energy. As we explained before, increased glucose in the blood causes a feeling of thirst, and the increased glucose enters the urine, causing frequent urination. Furthermore, the body begins to break down fatty tissues and release fatty acids in an effort to produce more fuel. These fatty acids are metabolized into chemicals called ketones, increasing the acid level in the blood to dangerous levels (this is called ketoacidosis). Initial symptoms of diabetic ketoacidosis;
- Excessive thirst and urination
- dehydration
- weight loss
- Nausea, vomiting
- feeling of hunger
- Dryness and redness of the skin
- rapid breathing
- Stomach ache
- confusion
It manifests itself with symptoms such as: One of the clearest symptoms is that the breath smells like fruit or nail polish remover (acetone). Diabetic ketoacidosis is a medical emergency that requires immediate hospitalization.
What is type 2 diabetes?
It accounts for 90-95 percent of diabetes cases and occurs later in life in overweight people. In this type (formerly called adult-onset diabetes), beta cells continue to produce insulin, but either the amount has decreased or the body cells are resistant to insulin.
Most people with type 2 diabetes are obese. Type 2 diabetes develops gradually and is most often identified in adulthood. However, with the increase in obesity in childhood, this disease is seen in more and more children. Type 2 diabetes can generally be controlled with exercise, a proper diet, weight loss and oral medications, without the need for insulin therapy. Therefore, Type 2 diabetes is also called non-insulin dependent diabetes. However, many patients sooner or later require insulin therapy.
What are the symptoms of type 2 diabetes?
Type 2 diabetes usually occurs slowly over many years, and its symptoms may not be noticed at first. In fact, most people with Type 2 diabetes are revealed by a routine laboratory test that shows high glucose in the blood. With the increase in glucose level, many people also experience the other symptoms we mentioned earlier:
- Frequent urination
- Increased thirst and fluid consumption
- Feeling of hunger in advanced stages
- Losing weight even though the amount of eating increases
- blurred vision
- Weakness and fatigue
- Recurrent vaginal yeast infections
These are temporary symptoms, do not cause permanent damage and disappear when the glucose level in the blood is controlled. In some people, complications such as peripheral neuropathy (damage to the nerves in the hands and feet) or coronary heart diseases may occur as the first signs of diabetes. These complications can be controlled, but not eliminated.
Another possible initial symptom of diabetes is the (non-ketotic) hyperosmolar hyperglycemia syndrome. These can occur when the stress of an injury, a major illness such as a stroke, a heart attack, or a severe infection raises the amount of glucose in the blood excessively (over 600 mg/dL). Even if the amount of insulin is at a level that does not require excessive ketone production (as in ketoacidosis), this is not high enough to prevent high blood glucose and hyperosmolarity (literally, thickening of the blood), where there are high concentrations of sodium, glucose, and other molecules that draw water from the cells into the circulatory system.
Symptoms of hyperosmolar hyperglycemia syndrome include dry mouth, increased hunger, nausea or vomiting, and dry and burning skin. Severe dehydration, which can lead to drowsiness, confusion, and even loss of consciousness, worsens the situation. In extreme cases, the result can go as far as coma. In order to avoid death, it is imperative to start insulin therapy immediately and give large amounts of intravenous fluids. If you see any of these symptoms in a loved one, call your doctor or call an ambulance without delay.
How is diabetes treated?
When you learn that you have a chronic disease such as diabetes, you will rightfully be depressed. However, the positive side is that diabetes is a disease that responds very well to treatment. Moreover, when you tell people around you that you have diabetes, you will be surprised to see how many people you know are in the same situation as you and generally live very normal, productive lives. Additionally, the tremendous amount of research being done on diabetes means that you will continue to encounter new treatment methods in the coming years.
Purpose of diabetes treatment
The aim of diabetes treatment is to keep your blood sugar and other risk factors (such as cholesterol and blood pressure) under control and to prevent long-term complications from occurring. The extent to which you can achieve this goal will vary depending on your age, weight, nutrition and exercise habits, work schedule, previous health problems, and whether your diabetes is Type 1 or Type 2. You will need to implement a personal treatment plan that takes all factors into consideration, and you will need to have patience and determination to follow this plan regularly. For many diabetics, this means constantly monitoring blood sugar levels, restricting certain foods, losing weight, and taking medications by mouth or injection.
Which doctor should be consulted for diabetes?
Your family doctor will likely determine various aspects of your diabetes treatment—but don’t assume he or she will do it alone. Although basic healthcare for people with diabetes is more complex, it is more appropriate to seek help from a professional team that specializes in various aspects of the disease. The captain of your ideal team is a good family doctor—a general physician or internist—with experience in treating diabetes. In some cases, especially in Type 1 diabetes, you may need a certified endocrinologist—a doctor with special training and expertise in conditions caused by abnormalities of hormone secretion (remember that insulin is a hormone). Whether you seek treatment from a general practitioner or a specialist depends on your particular situation and which one you have access to. “It always takes concrete evidence,” which means getting checked regularly—passing an A1c test, for example—and feeling good. If you don’t get regular checkups or your doctor doesn’t seem to take diabetes seriously, you need to look for another way. However, if your A1c values are normal and your condition is getting better, then you should definitely not leave your doctor.