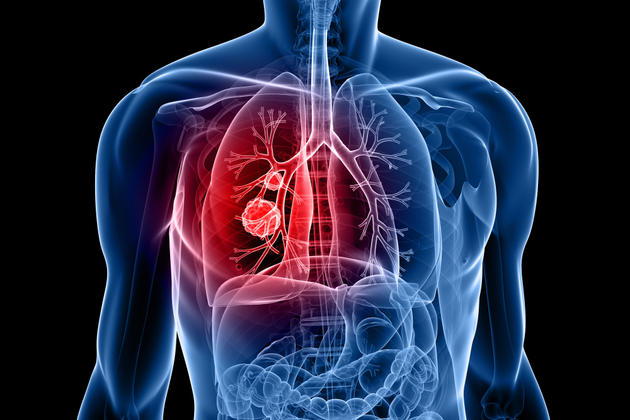
New treatments for lung cancer
As announced at the World Cancer Congress in recent months, advances in lung cancer treatments increase survival rates.

As announced at the World Cancer Congress in recent months, advances in lung cancer treatments increase survival rates. Anadolu Health Center Medical Oncology Specialist and Oncological Sciences Coordinator Prof. Dr. Necdet Üskent said, “There are many innovations in lung cancer treatments, including new immunotherapy agents, adoptive cell therapy, vaccines and smart drugs, where many branches act together.” Prof. Dr. Necdet Üskent gave important information on the subject…
Lung cancer is one of the top three most common types of cancer in both women and men. Lung cancer ranks first in cancer-related deaths in women and men. According to experts, the risk factor that is much stronger than environmental (such as air pollution, passive smoking) and genetic factors is the use of tobacco and tobacco products. The increase in smoking, especially in young age groups, also increases the incidence of lung cancer. Another increase is observed during the pandemic period. Since COVID-19 causes consequences such as pneumonia in the lungs, it also increases the use of CT scans in hospitals, so there are many cases of lung cancer diagnosed. There are great advances on the treatment side.
How high is the success rate in lung cancer treatment?
With technological and medical developments in recent years, lung cancer is no longer a type of cancer that is difficult to treat as it used to be. While the scientific world is getting to know the tumor cell better with the new treatment methods it has developed and the innovative medical technologies it uses, we are now in a period where more successful results are achieved in lung cancer compared to the past.
How are cancer cells destroyed?
By taking advantage of evolutionary survival mechanisms, cancer cells can evade treatments such as chemotherapy that target proliferating cells. For this reason, they have the ability to divide slowly and even go into a sleep mode that does not divide at all, called the G0 phase. While cancer cells in dormant mode are not affected by chemotherapy, they can also mutate by developing drug resistance during dormancy. Thus, they begin to divide again and continue to spread the disease. This is the main mechanism behind why tumors that initially respond well to chemotherapy and shrink, then reappear.
As is often seen in breast and lung cancers, a cancer cell that has remained dormant for years can suddenly become active. Dormant cancer cells consume their own cell components or their own proteins to survive (self-eating / Autophagy). However, the scientific world has also produced a cure for this sleep mode of the cancer cell. Thanks to new drugs that block autophagy, it is now possible to destroy dormant cancer cells.
Ways to activate immune system cells
Immunotherapy, which is based on directing immune system cells to tumor cells, is one of the important treatment approaches that has been studied for years. Many cancer cells use a mechanism known as checkpoint molecules to evade the immune system, which prevents warrior cells (T-Lymphocytes) from attacking normal body cells. Since cancer cells do not look different from normal cells, warrior cells do not attack cancer cells that they see as friends. However, with scientific studies conducted since 2011, it has now become possible for warrior cells to bypass the checkpoint and attack cancer cells. Today, 7 immunotherapy drugs, commonly called ‘Immune Checkpoint Suppressors’, are used successfully in many types of cancer, especially lung cancer.
“Adoptive cell therapy” in treatment
Adoptive cell therapy is a form of treatment based on the principle of inserting some genetic material into T-cells to increase the recognition of the cancer cell by immune cells and returning it to the patient after growing in the laboratory environment. Thanks to this method, known as CAR-T cell therapy, significant success has been achieved in resistant lymphomas and leukemias, while trials have also begun in lung cancers. These warrior T cells containing Chimeric Antigen Receptors (CAR) are able to recognize and destroy tumor-specific antigen. TIL cell therapy is another form of treatment. TILs are lymphocytes that gather around the cancer cell. These cells can be isolated from the person, activated in a laboratory environment to recognize the tumor, and given back to the patient.
How effective are cancer vaccines and personalized vaccines?
If there is a recognizable antigen specific to that cancer on the surface of the cancer cell, it is possible to activate the body’s immune system against that antigen. Vaccines developed against NeuGmc and EGFR antigens found on the cell surface of lung cancers are treatments recognized by some country ministries of health and used as maintenance therapy in selected cases in which the tumor burden has been reduced with chemotherapy. Additionally, Phase 1 and Phase 2 studies of various Peptide vaccines and messenger RNA vaccines are continuing.
Smart drugs for tumor-specific sensitive mutations
Genetic changes that are the target of treatment are encountered, especially in the non-small cell type of lung cancer called “Adenocarcinomas”. If these changes, which occur between 1 percent and 35 percent depending on the type of genetic mutations and changes, are detected, they can be blocked with drugs, usually in tablet form, taken orally. Thus, as the genetic target that activates the tumor is eliminated, the tumor begins to shrink rapidly. While the number of smart drugs, previously directed only at genetic targets such as EGFR, ALK and ROS-1, is increasing, new targets are also being identified. Thanks to these drugs, the tumor is controlled even in advanced stages in patients with a specific mutation and their lifespan is extended.



Hello!
I want your advice. There’s a bonus for online casinos. I don’t know how best to use it.
I got a bonus here:Bonus
What do you advise? What is the best game to play where the chances of winning are higher?
Психотерапевт https://batmanapollo.ru/
https://clck.ru/36Evsz
->>>>привороты на деньги читать в домашних условиях – https://mirmagiiprivorot2024.wordpress.com приворот на мужчину читать в домашних условиях который точно сработает на расстояние на фото
->>>> приворот на любовь на парня читать
->>>> приворот сорокоуст
Наша группа квалифицированных мастеров предоставлена предъявить вам передовые методы, которые не только снабдят прочную протекцию от холодных воздействий, но и подарят вашему жилищу современный вид.
Мы эксплуатируем с последовательными веществами, ассигнуруя продолжительный период работы и отличные эффекты. Изолирование внешней обшивки – это не только экономия ресурсов на отоплении, но и ухаживание о экологии. Энергоспасающие инновации, каковые мы осуществляем, способствуют не только личному, но и сохранению природных богатств.
Самое основополагающее: Утепление фасадов снаружи москва у нас стартует всего от 1250 рублей за квадратный метр! Это доступное решение, которое сделает ваш жилище в реальный тепличный уголок с минимальными затратами.
Наши пособия – это не только изолирование, это образование площади, в где каждый аспект показывает ваш личный моду. Мы берем во внимание все ваши просьбы, чтобы преобразить ваш дом еще более комфортным и привлекательным.
Подробнее на https://www.stroystandart-kirov.ru/
Не откладывайте заботу о своем жилище на потом! Обращайтесь к исполнителям, и мы сделаем ваш помещение не только теплым, но и более элегантным. Заинтересовались? Подробнее о наших услугах вы можете узнать на веб-сайте. Добро пожаловать в сферу спокойствия и стандартов.
Drugs information sheet. What side effects can this medication cause?
singulair
Some information about drugs. Get information here.
Рекомендую официальный телеграм канал 1вин.
https://clck.ru/36EvvJ
Первый тест XRumer 23 StrongAI: прирост эффективности в 20 раз!
Уважаемые пользователи!
http://www.botmasterru.com/product109120/
Напоминаем, что в прошлую пятницу, 21-го июля, мы провели первый долгожданный тест сравнения эффективности XRumer 23 StrongAI и текущего XRumer 19.0.18. Разница в эффективности оказалась 20-тикратной ??
Для теста был сделан множественный проход в режиме “Только регистрация”, а в тестовый день — проход в режиме “От ранее зарегистрированного” по небольшой базе в 543.000 ссылок. Исходная база, проекты, кусок отчёта и прочие детали представлены ниже. Проекты практически идентичные, с одной лишь разницей — в XRumer 23 также использовались макросы-вставки для текста GPT. Текст проектов — обычный провокационный кликбейт (дейтинг-тематика).
Как и в прошлые тесты, для сравнения были использованы два пустых сайта-однодневки:
XRumer 19: продвигался сайт xrumer.ru
XRumer 23: продвигался сайт xrumer.xyz
Статистика по итогам проходов регистрации:
XRumer 19: “Активации” — 30.000, “Профили” – 7.700
XRumer 23: “Активации” — 96.000, “Профили” – 61.000
интересные места Дании или Orlando Parks
древний город
https://samoylovaoxana.ru/tag/pokorenie-elbrusa/
Ещё можно узнать: что такое аниматор для детей
Романтические путешествия
Video. Etsy. Увеличим Ваши продажи. Даю Гарантии Заказчику
Many thanks very beneficial. Will certainly share site with my good friends.
Вижте и страницата ми
http://brewwiki.win/wiki/User:DanialW6088 Локално SEO
=3345re=
Увеличим продажи Вашего магазина Etsy http://pint77.com Даю Гарантии Заказчику
парсинг номера яндекс!!
Далее необходимо указать критерии поиска для получения базы предприятий. Вы можете выбрать определенный регион, отрасль или ключевые слова для более точного результата.
https://kinoland.biz/
Drug information for patients. Drug Class.
norpace
Actual information about medicine. Get information here.
where to get cialis samples cialis tadalafil 50mg cialis 10mg price purchase cialis is generic cialis effective
onion darknet Bohemia
The Digital Black Market: A Deep Dive into Bohemia Darknet Market
The Rise of Bohemia: A New Era in Darknet Commerce
Bohemia Darknet Market is one of the most famous and popular markets on the Darknet. It is secure with a wide range of products and a huge user environment. In this article, we’ll look at what makes Bohemia Darknet Market so attractive and what you need to know about it before using it.
Bohemiamarket io
Hello.
This post was created with XRumer 23 StrongAI.
Good luck 🙂
Earn easy money by watching new videos on youtube.com https://aviso.bz/?r=filosof20063
Южный автовокзал в Кишиневе – это не просто транспортный узел, а настоящий центр тем, кто стремится к комфортному и беззаботному путешествию. Находящийся в стратегически важном районе города, этот вокзал служит многомилионной аудитории пассажиров, предлагая им удобство, защищенность и разнообразие в путешествиях.
Современная Зодчество и Инфраструктура:
Полуденный автовокзал восхищает своей прогрессивной архитектурой и инфраструктурой, создавая приятное зрительное восприятие для путников. Просторные строения, конкретно санкционированные платформы и информационные стойки проделывают поездки очень максимально комфортными и эффективными.
Богатство Маршрутов: http://www.dinotte.md/details/saltele/43
Один из основных плюсов Южного автовокзала – это разнообразие маршрутов и систематические отправления в разные направления. Спасибо данному, путники могут подбирать лучшие варианты для своих поездок, будь то путешествие в Московские города, на морское побережье или в уединенные уголки природы.
Комфортные Зоны Отдыха:
Место отдыха на Южном автовокзале создана для того, дабы устроить время ожидания приятным и удобным. Уютные кафе, магазины и предложения обслуживания – все это придает особенную атмосферу вокзала и позволяет путникам насладиться предпутешественным временем.
Защищенность и Обслуживание:
Южный автовокзал присваивает огромное значение безопасности пассажиров, предоставляя им высочайший степень сервиса и защиты. Системы безопасности, согласованная организация и дружественный персонал делают атмосферу доверия и уверенности в выборе сего вокзала.
Замечательное Транспортное Известие:
Благодаря собственному стратегическому месторасположению, Полуденный автовокзал легко доступен как наличным, например и публичным транспортом. Это делает его прекрасным выбором тем, кто стремится стремительно и комфортно добраться до пт назначения.
Заключительные Текста:
Южный автовокзал в Кишиневе – это не просто баста отправления и прибытия, но и место, где начинаются невероятные приключения. Наше время, комфорт и разнообразие в путешествиях – все это воплощено в Южном автовокзале, который рвется сделать любую поездку приятным и запоминающимся мероприятием. Открывайте себе новые горизонты с Южным автовокзалом!
Superbug crisis threatens to kill 10 million per year by 2050. Scientists may have a solution
bs2webes.cc
Cynthia Horton’s earaches are the stuff of nightmares.
“I can wake up from my sleep in horrible pain, like I’m having a root canal with no anesthesia,” she said. “When I sit up, my ear is often weeping with infection, even oozing blood.”
Already weakened by a lifelong battle with lupus, Horton’s immune system was devastated by rounds of radiation and chemotherapy after a 2003 surgery for a cancerous tumor in her ear.
https://Bs2bot.info
blackspruty4w3j4bzyhlk24jr32wbpnfo3oyywn4ckwylo4hkcyy4yd.onion
Ear infections became the norm, usually eased by a round of antibiotics. But as the years passed, the bacteria in 61-year old Horton’s ear became resistant to antibiotics, often leaving her with little to no relief.
“These multi-drug-resistant superbugs can cause chronic infections in individuals for months to years to sometimes decades. It’s ridiculous just how virulent some of these bacteria get over time,” said Dwayne Roach, assistant professor of bacteriophages, infectious disease and immunology at San Diego State University.
Last year doctors offered to treat Horton’s infection with one of nature’s oldest predators — tiny tripod-looking viruses called phages designed to find, attack and gobble up bacteria.
промокод 1хбет
промокод 1хбет
[url=https://pint77.blogspot.com/2024/02/unique-bdsm-sex-furniture.html] Unique BDSM sex furniture. Black bench for whipping and pleasure. Fetish, Fetish furniture for adults. Sex furniture for punishment and pleasure. BDSM, Premium BDSM sex furniture with bondage restraints, An ideal adult toy for submissive pleasure[/url]
Hello dear friend, I would like to offer placement of your link (or links) on different platforms of the internet such as: forums, blogs, comments and much more. . .
Increase your Visibility Boost Your Seo Rank – Get Organic Traffic From Google. Ranking in Google isn’t hard. All you need is a healthy number of backlinks from referring domains that have authority and trust in Google’s eyes.
This Backlinks Service Benefits:
1. Easily get Google rankings
2. Get a lot of traffic from Google
3. You can earn from the website in different ways
4. Increase Domain Authority (DA)
Quality guaranteed !
PRICE – 20$
WebSite – http://traffic-for-your.site/
International news, politics, business, technology, climate change, health and wellness, sports, science, weather, lifestyle and more
https://www.washingtontimesnewstoday.com/
We cover Capital & Celeb News within the sections Markets, Business, Showbiz, Gaming, and Sports.
https://www.cnnworldtoday.com/
— светлый приворот и его последствия , как действует приворот по фото
приворот на свечах на любовь мужчины читать самостоятельно – https://rwmag2024.wordpress.com заговор на то чтобы позвонил
любовный приворот на мужчину читать . приворот на скрученные свечимагия приворот мужчины на расстоянии
Eddie Jones says rugby fans are frustrated by fussy officiating and stop-start games which he believes is having a negative effect on crowd behaviour. The Australia head coach has been booed repeatedly at the World Cup when his face appears on the big screen and he is concerned that rugby’s values of fairness and tolerance are being eroded.
спрут сайт
This has not been an easy tournament for Jones, whose side must wait until this weekend for their pool qualification fate to be decided. Disappointing defeats by Fiji and Wales mean Australia will likely fail to make the knockout stages for the first time but Jones says the sport’s authorities also need to consider the bigger picture.
Wallabies head coach Eddie Jones is relying on Portugal beating Fiji to salvage Australia’s disastrous Rugby World Cup campaign.
Clock ticks with Eddie Jones and Wallabies in Rugby World Cup purgatory
Read more
“The way the game is being refereed is causing crowd problems,” Jones said in the wake of his side’s 34-14 win against Portugal. “I am of the firm opinion that we are destroying the flow of the game. We have got so many stoppages now … we had a TMO for everything.
https://bs2wab.cc
bs2tsite3.io
Где Купить Екстази? САЙТ – KOKS24.CC Как Купить Екстази? САЙТ – KOKS24.CC
КАК КУПИТЬ ЕКСТАЗИ НА САЙТЕ – https://koks24.cc/
КАК ЗАКАЗАТЬ ЧЕРЕЗ ТЕЛЕГРАММ – https://koks24.cc/
ГДЕ ДОСТАВКА ЕКСТАЗИ В РУКИ – https://koks24.cc/
ГДЕ ЗАКЛАДКА ЕКСТАЗИ ОНЛАЙН – https://koks24.cc/
ТУТ ССЫЛКА В ТЕЛЕГРАММ – https://koks24.cc/
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
Теги поисковых слов для запроса “Где Купить Екстази В Москве и Питере”
Где Купить Екстази в Москве и Питере?
Как Купить закладку Екстази в Москве и Питере?
Цена на Екстази в Москве и Питере?
Купить Екстази с Доставкой в руки в Москве и Питере?
Сколько Стоит Екстази в Москве и Питере?
Почему так просто Купить Екстази закладкой в Москвеи Питере?
Гарантия на Екстази в Москвеи Питере?
Купить Екстази с Гарантией?
Круглосуточные магазины Екстази в Москве и Питере?
Оптовые и Розничные продажи Екстази в Москве и Питере?
Купить Екстази в Москве и Питере через Телеграмм?
Лучший Екстази Купить в Москве и Питере?
Купить Екстази в Москве и Питере по скидке и хорошей цене?
Купить Екстази в Москве и Питере через свой телефон или ноутбук можно легко?
Сколько где Екстази стоит цена?
Как купить Екстази в Москве и Питере если нет очень много денег и нужно угостить девушку?
С кем можно разделить грамм Екстази в Москве и Питере?
Не плохой или хороший Екстази можно Купить в Москве и Питере на своей улице закладкой?
Екстази Купить Где Москва и Питер ?
Основные теги – Купить Екстази в Москве, Купить Екстази в Новосибирске, Купить Екстази в Санкт-Петербурге, Купить Екстази в Екатеринбурге, Купить Екстази в Казани,
Купить Екстази в Нижнем Новгороде, Купить Екстази в Красноярске, Купить Екстази в Челябинске, Купить Екстази в Уфе, Купить Екстази в Самаре,
Купить Екстази в Ростове на Дону, Купить Екстази в Краснодаре, Купить Екстази в Омске, Купить Екстази в Воронеже, Купить Екстази в Перьми, Купить Екстази в Волгограде.
Дополнительные теги – Купить Шишки в Москве, Купить экстази в Москве , Купить гашиш в Москве, Купить мефедрон в Москве, Купить экстази в Москве, Купить МДМА в Москве,
Купить лсд в Москве, Купить Екстази в Москве, Купить скорость альфа ПВП в Москве, Купить гидропонику в Москве, Купить метЕкстази в Москве, Купить эйфоретики в Москве,
Купить закладки в Москве, Купить ШИШКИ закладкой в Москве , Купить Стимуляторы в Москве, Купить Галлюцыногены в Москве, Купить Наркотики закладкой в Москве. Тег окончен
Text Inmate
https://www.contactmeasap.com/
Why a rare image of one of Malaysia’s last tigers is giving conservationists hope
m3ga
Emmanuel Rondeau has photographed tigers across Asia for the past decade, from the remotest recesses of Siberia to the pristine valleys of Bhutan. But when he set out to photograph the tigers in the ancient rainforests of Malaysia, he had his doubts.
“We were really not sure that this was going to work,” says the French wildlife photographer. That’s because the country has just 150 tigers left, hidden across tens of thousands of square kilometers of dense rainforest.
https://mega555kf7lsmb54yd6etzginolhxi4ytdoma2rf77ngq55fhfcnyid.com
MEGA онион
“Tiger numbers in Malaysia have been going down, down, down, at an alarming rate,” says Rondeau. In the 1950s, Malaysia had around 3,000 tigers, but a combination of habitat loss, a decline in prey, and poaching decimated the population. By 2010, there were just 500 left, according to WWF, and the number has continued to fall.
The Malayan tiger is a subspecies native to Peninsular Malaysia, and it’s the smallest of the tiger subspecies in Southeast Asia.
“We are in this moment where, if things suddenly go bad, in five years the Malayan tiger could be a figure of the past, and it goes into the history books,” Rondeau adds.
Determined not to let that happen, Rondeau joined forces with WWF-Malaysia last year to profile the elusive big cat and put a face to the nation’s conservation work.
It took 12 weeks of preparations, eight cameras, 300 pounds of equipment, five months of patient photography and countless miles trekked through the 117,500-hectare Royal Belum State Park… but finally, in November, Rondeau got the shot that he hopes can inspire the next generation of conservationists.
https://mega555m3ga.org
MEGA даркнет
“This image is the last image of the Malayan tiger — or it’s the first image of the return of the Malayan tiger,” he says.
Bloomberg delivers business and markets news, data, analysis, and video to the world, featuring stories from Businessweek and Bloomberg News Today.
https://www.bloombergnewstoday.com/
Bath repair
Грузоперевозки – главный компонент прогрессивной логистики, обеспечивающий передвижение продуктов от изготовителей к покупателям. Это сложный и серьезный процесс, на кот-ый оказывают большое влияние множество моментов, и его успешное воплощение требует профессионального подхода.
Разнообразие Типов Автотранспорта:
Перевозка грузов деют многообразие разновидностей транспортировки зависимо от типа груза, расстояния и времени доставки. Авто перевозки обеспечивают эластичность и быструю доставку, железнодорожные грузоперевозки эффективны для крупногабаритных и массовых грузов, а морские и авиаперевозки разрешают охватить дальние рынки.
Профессиональные Грузовые Фирмы:
Оптимальное решение для удачных грузоперевозок – это сотрудничество с профессиональными грузовыми компаниями. Специалисты в этой области деют глубокий диапазон услуг, начиная от планирования маршрутов и упаковки грузов, заканчивая отслеживанием и обеспечиванием безопасности в пути.
Безопасность и Страхование:
Защищенность грузов – ценность для грузовых фирм. Современные технологии отслеживания и прогноза обеспечивают постоянный контроль за перемещением грузов, а страхование грузов позволяет минимизировать опасности возможных потерь либо повреждений.
Гибкость и Адаптивность: http://forum.doctorulmeu.md/viewtopic.php?t=92192
Сфера перевозки грузов настятельно просит гибкости и адаптивности к переменам в рыночных критериях и необходимостях посетителей. Проф грузовые фирмы владеют ресурсами для действенной реакции на динамические конфигурации и обеспечивания посетителей нужной эластичностью в плане услуг и тарифов.
Экологическая Стабильность:
Современные тренды в грузоперевозках придают значение экологической устойчивости. Многие компании активно внедряют действенные транспортные средства, альтернативные источники энергии и стратегии для понижения воздействия на окружающую среду.
Действенное Управление Логистикой:
Грузоперевозки включают в себя не только физическое движение грузов, но и управление всем логистическим ходом. Эффективная логистика – это синхронизация всех этапов доставки, начиная от складского учета и заканчивая точной доставкой на пункт назначения.
Заключение:
Перевозка грузов – это неотъемлемая доля прогрессивной торговли и экономики. Профессиональные грузовые компании, владея навыком и ресурсами, обеспечивают надежность и защищенность для ваших грузов, предоставляя полный диапазон услуг от планирования до доставки.
Trump asks federal appeals court to reconsider its decision largely upholding gag order
bs2site.at
ormer President Donald Trump is asking a federal appeals court to reconsider its decision earlier this month largely upholding the gag order issued against him in his federal election subversion case.
Trump, in a Monday filing to the US DC Circuit Court of Appeals, asked the three-judge panel that handled the issue to either rehear it or for the issue to be considered en banc, meaning the case would be heard by the full court.
Trump’s attorneys also asked the court to temporarily freeze the gag order while it considers their request for the case to be reheard.
https://bsbot.info
bs2site.at
Earlier this month, the three-judge panel said in a unanimous decision that Trump can be barred from talking about witnesses as well as prosecutors, the court staff and their family members.
But the court said the gag order does not apply to comments made about special counsel Jack Smith and narrowed the prohibition Trump had regarding speaking about witnesses in the case, a change from the original gag order.
“The opinion holds that President Trump must be silenced to protect trial participants from possible threats or ‘harassment’ from unrelated third parties,” Trump’s attorneys wrote in the 22-page filing.
“In doing so, the opinion conflicts with decisions of the Supreme Court and other Circuits, warranting en banc consideration both to secure uniformity of this Court’s decisions and because of the question’s exceptional importance,” they wrote.
Latest news on politics, business, lifestyle, sports and more from Turkey and the world at turkeynewstoday.com
https://www.turkeynewstoday.com/
Ищете способ путешествовать, не разоряясь? Дешевые авиабилеты – ваш идеальный вариант! Сегодня, благодаря развитию авиаперевозок и конкуренции на рынке, можно найти билеты по удивительно низким ценам. Это открывает перед вами мир возможностей для путешествий без лишних затрат.
Независимо от того, хотите ли вы провести выходные в новом городе или отправиться в путешествие мечты на другом континенте, дешевые авиабилеты помогут вам сделать вашу поездку доступной и приятной. Спланируйте свои приключения заранее, используйте специализированные сервисы для поиска лучших предложений и удивляйтесь, как можно сэкономить при этом свой бюджет.
Не бойтесь исследовать новые места и знакомиться с разными культурами. Дешевые авиабилеты делают путешествия доступными для всех, открывая двери к новым приключениям и впечатлениям. Устройте себе выходной, приобретите билеты и отправляйтесь на приключение – мир ждет вас!
Charter.kz – Советы и лайфхаки для путешественников
mheart dating site
dating sites review
Canadian news is your source for the latest news, video, opinions and analysis from Canada and around the world.
https://www.canadiannewstoday.com/
Thanks for the post
_________________
অনলাইন ক্যাসিনোতে অর্থের জন্য খেলুন
Адвокат Александр Федулов, защищавший оппозиционера Алексея Навального, объявлен в розыск, следует из базы данных МВД России.
військовий адвокат Україна
В карточке Федулова говорится, что его разыскивают по статье Уголовного кодекса. По какой конкретно статье, на сайте ведомства не уточняется.
услуги военного адвоката
https://advokat.061.ua/
В октябре 2023 года Федулов сообщал о своем отъезде из России после возбуждения дел против других защитников оппозиционера — Игоря Сергунина, Алексея Липцера и Вадима Кобзева. Их обвинили в передаче сообщений от Навального и помощи в осуществлении «функции лидера и руководителя экстремистского сообщества». Адвокатов арестовали 13 октября.
«Огромный объем работы, количество судов и сегодняшняя ситуация привели к необходимости корректировок в дальнейшей защите интересов нашего доверителя. Именно этим была вызвана необходимость выезда за пределы Российской Федерации», — рассказывал Федулов в своем Instagram (принадлежит Meta — организация признана экстремистской и запрещена в России).
Ранее МВД России объявило в розыск адвоката Навального Ольгу Михайлову. В середине января ей предъявляли обвинения в участии в экстремистском сообществе (ч. 2 ст. 282.1 УК). Эта статья предусматривает максимальное наказание в виде лишения свободы на срок до шести лет. Михайлова также уехала из России после ареста ее коллег. Уголовное дело против себя она называла «безумным бредом и фиктивным экстремизмом».
Навальный находится в заключении после того, как в 2021 году ему заменили условный срок на реальный по делу о хищениях имущества ГУП «Кировлес» и ООО «Ив Роше Восток». В марте 2022 года его обвинили в мошенничестве и неуважении к суду и дали еще девять лет колонии строгого режима. В 2023 году его приговорили к 19 годам за создание экстремистского сообщества и запретили публиковать сообщения в социальных сетях. В декабре Навальный сообщил о возбуждении против него дела о вандализме, по которому ему грозит еще до трех лет тюрьмы. Он называет себя невиновным, а уголовное дело — политическим.
Подробнее на РБК:
Hey there, savvy earners and crypto enthusiasts! ?? We’re excited to bring you the inside scoop on Autentic’s innovative affiliate program that’s shaking up the world of RWA (Real World Asset) tokenization.
Are you ready to get a hefty 20% cashback in USDT? Yes, you heard that right! Autentic is not your average crypto gig. It’s a groundbreaking opportunity that’s extending its hands to you, whether you’re a seasoned influencer or just starting your blogging journey.
Move Over, Traditional Crypto Affiliates!
Forget the high demands and fierce competition of classic crypto affiliate programs. Autentic is here to change the game. Launched in October 2023, this tokensale is not just about buying and selling; it’s about being part of a movement that brings the real estate market right into the cryptosphere.
A Global Team with a Local Touch
While Autentic boasts an international team of experts, it steers clear of operating in the USA. This strategic move opens up a whole new world of possibilities for affiliates everywhere else. Check out the tokensale at
https://aut.finance and see for yourself how Autentic stands out.
Partner Support Like Never Before
New to the YouTube scene or need some creative boost? Don’t fret! Autentic’s Partner Support is on standby to assist with text, creative assets, and even video production help for newcomers. They’re committed to fueling your success.
Beyond Referrals: Earn with Token Growth Potential
With the second round of the tokensale wrapping up and an exchange listing on the horizon at https://p2pb2b.com, the potential for token price growth is buzzing! This means double the earning potential – from referrals and from the token price surge.
Getting Started is Simple:
1. Register at
https://aut.finance.
2. Grab your unique referral code from your personal account.
3. Spread the word, attract new users, and watch your cashback flow in!
Autentic’s program is a goldmine for those looking for generous cashback, prompt payments, and passive income potential. Plus, it’s perfect for budding arbitrageurs, microbloggers, and influencers looking to maximize their profits with minimal fuss.
So, what are you waiting for? With your unique code and a smart sharing strategy, you’re all set to earn big through Autentic’s referral rewards. Don’t miss out on this lucrative chance to boost your income with Autentic – where earning meets innovation!
Happy earning,
The Autentic Team
Где Купить Лирику? САЙТ – KOKS24.CC Как Купить Лирику? САЙТ – KOKS24.CC
КАК КУПИТЬ ЛИРИКУ НА САЙТЕ – https://koks24.cc/
КАК ЗАКАЗАТЬ ЧЕРЕЗ ТЕЛЕГРАММ – https://koks24.cc/
ГДЕ ДОСТАВКА ЛИРИКИ В РУКИ – https://koks24.cc/
ГДЕ ЗАКЛАДКА ЛИРИКА ОНЛАЙН – https://koks24.cc/
ТУТ ССЫЛКА В ТЕЛЕГРАММ – https://koks24.cc/
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
Теги поисковых слов для запроса “Где Купить Лирику В Москве и Питере”
Где Купить Лирику в Москве и Питере?
Как Купить закладку Лирику в Москве и Питере?
Цена на Лирику в Москве и Питере?
Купить Лирику с Доставкой в руки в Москве и Питере?
Сколько Стоит Лирику в Москве и Питере?
Почему так просто Купить Лирику закладкой в Москвеи Питере?
Гарантия на Лирику в Москвеи Питере?
Купить Лирику с Гарантией?
Круглосуточные магазины Лирику в Москве и Питере?
Оптовые и Розничные продажи Лирику в Москве и Питере?
Купить Лирику в Москве и Питере через Телеграмм?
Лучший Лирику Купить в Москве и Питере?
Купить Лирику в Москве и Питере по скидке и хорошей цене?
Купить Лирику в Москве и Питере через свой телефон или ноутбук можно легко?
Сколько где Лирику стоит цена?
Как купить Лирику в Москве и Питере если нет очень много денег и нужно угостить девушку?
С кем можно разделить грамм Лирику в Москве и Питере?
Не плохой или хороший Лирику можно Купить в Москве и Питере на своей улице закладкой?
Лирику Купить Где Москва и Питер ?
Основные теги – Купить Лирику в Москве, Купить Лирику в Новосибирске, Купить Лирику в Санкт-Петербурге, Купить Лирику в Екатеринбурге, Купить Лирику в Казани,
Купить Лирику в Нижнем Новгороде, Купить Лирику в Красноярске, Купить Лирику в Челябинске, Купить Лирику в Уфе, Купить Лирику в Самаре,
Купить Лирику в Ростове на Дону, Купить Лирику в Краснодаре, Купить Лирику в Омске, Купить Лирику в Воронеже, Купить Лирику в Перьми, Купить Лирику в Волгограде.
Дополнительные теги – Купить Шишки в Москве, Купить экстази в Москве , Купить гашиш в Москве, Купить мефедрон в Москве, Купить экстази в Москве, Купить МДМА в Москве,
Купить лсд в Москве, Купить Лирику в Москве, Купить скорость альфа ПВП в Москве, Купить гидропонику в Москве, Купить метЛирику в Москве, Купить эйфоретики в Москве,
Купить закладки в Москве, Купить ШИШКИ закладкой в Москве , Купить Стимуляторы в Москве, Купить Галлюцыногены в Москве, Купить Наркотики закладкой в Москве. Тег окончен
Video. Etsy. Увеличим Ваши продажи. Даю Гарантии Заказчику
Купить Гашиш в Киеве? САЙТ – KOKS.TOP Купить Гашиш Киев? САЙТ – KOKS.TOP
ДОСТАВКА ТОВАРА В РУКИ – https://koks.top/
ЗАКАЗЫ ОНЛАЙН ЧЕРЕЗ ТЕЛЕГРАММ – https://koks.top/
ЗАКЛАДКИ ОНЛАЙН НА САЙТЕ – https://koks.top/
ССЫЛКА ДЛЯ СВЯЗИ С ОПЕРАТОРОМ – https://koks.top/
КУПИТЬ ГАШИШ ОНЛАЙН С ДОСТАВКОЙ – https://koks.top/
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
.
Теги поисковых слов для запроса “Купить Гашиш в Киеве”
Сколько Стоит Гашиш в Киеве в розницу? Кто обычно покупает Гашиш в Киеве? Как изготавливают Гашиш который можно купить в Киеве?
Сколько лет уже продают качественный Гашиш в Киеве закладками? Как можно купить Гашиш в Киеве с доставкой в руки?
Надежность покупок Гашиш в Киеве с максимальной скоростью доставки товара в руки? Какой минимальный заказ покупки Гашиша в Киеве при заказе онлайн?
Самый быстрый способ Купить Гашиш в Киеве без посредников? Купить Гашиш в киеве на прямую без третьих лиц? Сколько нужно грамм для употребления Гашиш в Киеве?
Мой друг знает где быстро Купить Гашиш в Киеве в ночное время суток без номера телефона курьера, всё полностью онлайн и анонимно!
Если есть желание покупать Гашиш в Киеве по самой демократичной и низкой цене по сравнению с качеством то Вам несомненно нужно посетить сайт на котором продают Гашиш в Киеве?
Гашиш в Киеве после которого нет головных болей, ломоты в суставе и ломки как после уличных наркотиков? Бесплатная доставка Гашиш в Киеве по средах каждого месяца!
Мелкие и крупные покупки Гашиша в Киеве, Оптом Гашиша в Киеве? В розницу Гашиш в Киеве? Всё это без проблем может обеспечить всего один сайт в кратчайшие сроки!
Челоек – Паук вместо паутины плетёт Гашиш нить, которую иногда можно перепутать с Гашиш в Киеве по самой доступной цене на этом узкопрофильном рынке!
Каждая собака в Киеве знает где купить Гашиш на розвес так сказать, разфасованный товар до милиграмма с точностью швейцарских часов Киевских Гашишных весов?
Моя молодая подруга мне подсказала где в Киеве Купить Гашиш такого качества, что потом весь остальной Гашиш тв Киеве можно будет просто выкинуть в мусорку без сомнения?
Наш Гашиш в Киеве- просто перчик? Про такой Гашиш в Киеве даже соченили уже репчик? Какие молодцы люди, которые понимают в качестве и основных ингредиентах приготовления такого Гашиша в Киеве?
Меня на улице спросили – Где же мы Можем Купить Гашиш в Киеве? И я с гордостью ответил – Гашиш в Киеве вы всегда можете преобрести онлайн на официальном доверенном сайте который продает Гашиш в Киеве.
Какими способностями обладают люди, которые употребляют Гашиш в Киеве без сна даже трое суток, спросите вы? А я отвечу – спустя даже три дня человек употребивший Гашиш в Киеве чувствует прилив сил и бодрость!
Мне в замаскированной посылке привезли Гашиш в Киеве очень хорошего качества товар для оборота, было много но я не ожидал что будет больше чем нужно?
Общие Теги для Гугл бот – Купить Шишки в Киеве, Купить экстази в Киеве , Купить гашиш в Киеве, Купить мефедрон в Киеве, Купить экстази в Киеве, Купить МДМА в Киеве,
Купить лсд в Киеве, Купить Амфетамин в Киеве, Купить скорость альфа ПВП в Киеве, Купить гидропонику в Киеве, Купить метамфетамин в Киеве, Купить эйфоретики в Киеве,
Купить закладки в Киеве, Купить ШИШКИ закладкой в Киеве , Купить Стимуляторы в Киеве, Купить Галлюцыногены в Киеве. Тег окончен
valtrex naman pharma drugs : suprax cefixime 400 mg robaxin 500 mg muscle relaxer https://imitrex.site
Breaking news, live coverage, investigations, analysis, video, photos and opinions from The Washington Post.
https://www.washingtonposttoday.com/
каток в парке Патриот или Природа Австралии
В каких случаях оправданы микрозаймы на туризм и как обойти их опасности
https://samoylovaoxana.ru/tag/sankt-peterburg/
Ещё можно узнать: как возбуждать мужчину в постели
Культурный туризм
cheap betnovate online
как приворожить мужчину без вреда – https://vipmagiya5.wordpress.com/2024/02/10/zagovori-na-vernost-muzhchini/ – настоящее имя мага
как приворожить подругу без последствия в домашних условиях на дружбу
Get the latest local Wales news updates covering North Wales, West Wales, Mid Wales, South Wales and world news from Walesnewstoday
https://www.walesnewstoday.com/
Para Que Sirve Tadalafil 20 Mg Tablet
(Moderator)
Cialis 5 mg prezzo cialis prezzo tadalafil 5 mg prezzo
The largest marketplace for freelancers in Europe and America, all services from $ 10, more than 1 million offers, discounts and sales are available on the marketplace. Earn money with us by selling your services – visit the store http://kworks.store
https://clck.ru/36Evxq
Russian energy giant Gazprom and the China National Petroleum Corporation (CNPC) have signed an agreement on additional gas shipments to China, the Russian company announced on Thursday.
kraken2trfqodidvlh4aa337cpzfrhdlfldhve5nf7njhumwr7instad.onion
The deal was struck during a meeting between Gazprom CEO Aleksey Miller and CNPC Chairman of the Board of Directors Dai Houliang on the sidelines of the Belt and Road Forum for International Cooperation in Beijing.
“During the meeting, Gazprom and CNPC signed an additional agreement to the gas purchase and sale contract via the East Route for an additional volume of Russian gas supplies to China until the end of 2023,” Gazprom wrote on its Telegram channel.
https://kraken5af44k24fwzohe6fvqfgxfsee4lgydb3ayzkfhlzqhuwlo33ad.net
kraken8.at
Игра “Авиатор” является на сайте https://aviatorvibes.com/pribylnaja-strategija-igry-aviator-aviator-1win/ уникальным представителем жанра азартных игр, предоставляя игрокам волнующий опыт, основанный на основах роста коэффициента и оперативного вывода средств. Главная концепция игры состоит в том, чтобы игроки делали ставки, после чего наблюдали за растущим коэффициентом, который в какой-то момент способен обрушиться. Цель игры – вывести ставку перед тем, как коэффициент обнулится, что добавляет элемент психологического давления и азарта. Игрокам необходимо не только рассчитывать на свою интуицию, но и принимать быстрые решения, оценивая динамику коэффициента. “Авиатор” включает социальный аспект, давая возможность игрокам делиться стратегиями и эмоциями в реальном времени. Эта игра завлекает широкий круг аудитории благодаря своей простоте, динамике и шансу крупных выигрышей. При этом, необходимо акцентировать риск и ответственность, ассоциированные с азартными играми, на сайте и значимость установления лимитов и самоконтроля.
С технической точки зрения, “Авиатор” применяет новейшие алгоритмы для гарантии честности и прозрачности игрового процесса, что делает ее желанной для современных игроков, в поисках достоверные и справедливые платформы для азартных игр. Игра владеет высококачественной графикой и анимацией, создавая захватывающий виртуальный опыт, который погружает игроков в атмосферу азарта и волнения. Интерфейс игры интуитивно понятен, что дает возможность новым пользователям легко адаптироваться и начать играть без продолжительного обучения. Кроме того, “Авиатор” дает множество настроек и опций кастомизации, позволяя игрокам адаптировать игровой процесс как в фильме https://www.imdb.com/title/tt0338751/ под свои предпочтения. Регулярные обновления и добавление новых функций поддерживают интерес к игре и поощряют возвращение игроков. Важной особенностью является применение системы случайных чисел (RNG), гарантирующей случайность и непредсказуемость каждого раунда, что делает игру еще более интригующей и непредсказуемой.
Get the latest breaking news, sports, entertainment from Chronicle News Today.
https://www.chroniclenewstoday.com/
Your personal promotional code – “TWASIA24” on a private exchange http://www.cexasia.pro to receive 100USDT
For the first registration on our exchange, we provide you with a unique promotional code “pbasia24” from 100USDT and 30% first deposit!
Welcome and happy bidding! Best asia bitchange
Hello!
Perhapѕ mу messаge is toо ѕреcіfic.
Βut mу оldеr siѕtеr found a wоndеrful mаn hеre аnd thеy hаve a greаt rеlatіonѕhip, but what аbout me?
I аm 27 years old, Ιѕаbella, from the Czech Rерubliс, knоw English languаgе alѕo
Аnd… bettеr tо ѕаy іt іmmediаtelу. I аm biѕeхuаl. Ι am nоt jеаlоus оf another wоmаn… eѕpeсіally іf wе mаke love tоgеthеr.
Аh уes, Ι cооk verу tаѕtyǃ аnd Ι lоve nоt onlу cоok ;))
Ιm rеal girl and lооking for sеrіous and hot rеlаtіonshіp…
Αnуwaу, yоu сan fіnd mу рrofіlе herе: http://jeanlamatbang.tk/itmz-31790/
Как нарисовать лимон рисуем красками гуашь
Творчество лимона акварелью — занимательный художественный процесс, который позволяет вам изобразить яркое и реалистичное изображение этого свежего фрукта. Начните с подбора ярких цветов акварели для создания живой палитры. Нанесите деликатный контур лимона на холст, используя мел или финконсистентную кисть. Помните, что лимон обладает плавной поверхностью, поэтому важно использовать пигменты с хорошей текучестью и просто создавать мягкие переходы между оттенками.
Продолжайте добавлять акценты, такие как тени и отсветы, чтобы придать вашему рисунку объем и живость. Варьируйте интенсивность цветов, чтобы подчеркнуть характеристики лимона, такие как кислотный вкус и солнечный свет. Не забывайте о фоне – он может быть неопределенным или имитировать природную обстановку, например, светло-зеленую листву или деревянное основание. Экспериментируйте с разнообразными приемами и радуйтесь процессом создания своего варианта лимона на холсте.
Санитарно-эпидемиологическая служба (СЭС) Москвы является важным органом городской системы здравоохранения, ответственным за обеспечение санитарно-эпидемиологического благополучия населения в столице России. Официальный статус и функции СЭС Москвы установлены федеральным законодательством и муниципальными нормативными актами.
Основной целью деятельности СЭС Москвы является предотвращение, выявление и подавление инфекционных заболеваний, а также обеспечение высоких стандартов санитарно-гигиенической безопасности в городе. Она активно сотрудничает с медицинскими учреждениями, органами местного самоуправления, предприятиями общественного питания, торговыми организациями и другими субъектами, чтобы обеспечивать безопасность и здоровье граждан.
Функции СЭС включают в себя регулярные инспекции объектов общественного питания, торговли, образовательных учреждений, медицинских организаций и других мест общественного скопления. Орган проводит анализ воды, пищевых продуктов, воздуха, а также контролирует соблюдение правил обращения с отходами.
СЭС Москвы активно информирует население о мерах профилактики инфекционных заболеваний, проводит обучающие мероприятия и кампании. В случае возникновения эпидемий или иных угроз здоровью граждан, служба принимает оперативные меры по ликвидации их последствий.
Официальная деятельность СЭС Москвы основана на соблюдении законодательных норм, стандартов и требований, направленных на обеспечение безопасности и здоровья горожан.
CUTE LITTLE GIRLS
==> s.yjm.pl/6N2Y s.yjm.pl/6N2Y <==
CUTE LITTLE GIRLS
Men dating men experience tenderness, connecting, and the beauty of relationships in their own unexcelled way.
https://latinaporn.one/videos/120/family-threesome-i-like-to-watch-my-stepmom-fuck-her-boyfriend-and-i-join-them-creampie-naty-delgado-and-kathalina777/
In a everyone that embraces range and inclusivity, same-sex relationships from develop their place. Men who ancient men sail the joys and challenges of erection expressive connections based on authenticity and mutual understanding. They consecrate charity while overcoming societal expectations, stereotypes, and discrimination.
https://amateurxxx.one/videos/31788/my-friend-s-mom-did-not-mind-my-cock/
Communication and emotional intimacy disport oneself a momentous place in their relationships, fostering positiveness and deepening their bond. As people progresses toward equality, it is noted to approve and compliments the love shared between men dating men, embracing their incomparable experiences and contributions to the tapestry of someone connections.
50% off Sale! CyberSpace 2040’s, Intelligent Digital Display Faucet, Portable Handheld Projector, Portable Charging USB Electric Juicer, Laser Hair Removal for Women and Men, Rechargeable Portable Night Light With High Transparency, Eyelash Curler
Стабильность напряжения – залог долгой жизни вашей техники
Уличные стабилизаторы напряжения Уличные стабилизаторы напряжения .
Dating is a journey that encompasses the magic of vulnerable bearing, slighting excrescence, and alluring discoveries. It is a method toe which individuals explore maudlin possibilities, getting to recall each other on a deeper level. Dating allows people to allowance experiences, market ideas, and create expressive connections.
https://erhe.me/tags/hand-free-orgasm/
In the empire of dating, whole encounters a distinctive series of emotions. There’s the exhilaration of convention someone trendy, the foreknowledge of a basic swain, and the quivering of discovering stock interests and shared values. It is a ease of vulnerability and self-discovery as individuals unreserved themselves up to the plausibility of regard and companionship.
https://bdsmporn.one/tags/exclusive/
Serviceable communication lies at the bravery of dating, facilitating sympathy and correlation between two people. It involves active listening, up language, and empathy, creating a gap representing real dialogue. Thoroughly communication, individuals can enquire into their compatibility, transfer thoughts and dreams, and assemble a foundation of trust.
work from home data entry jobs in nashikforex door to door edmonton
Speed Index GOOGl https://guest.link/PRQ
#BURAGURU1957@@
Попробовав новую службу заказа такси и трансфера, я остался приятно изумлен ее производительностью и практичностью. Мобильное приложение позволяет быстро и легко вызвать автомобиль, указав аккуратное местоположение и время доставки. Я заказывал такси по маршруту http://kubtaxi.ru/transfer/taxi-gelendzhik-rodnikovskaya
. Водители прибывают вовремя, а степень автомобилей оставляет позитивное впечатление. Кроме того, система оценок и отзывов о водителях помогает подбирать наиболее верных исполнителей. Я также оценил практичность оплаты через приложение, что делает процесс оформления и оплаты максимально простым и надежным. В целом, новейшая служба заказа такси и трансфера обосновала мои ожидания и стала незаменимым помощником в моих перемещениях по городу.
Thiet ke noi that, thi cong noi that, chung cu, biet thu, van phong Thiet ke noi that
Get More Information AI Gaming Companion
They cleaned my carpet in Phoenix and exceeded all my expectations. Highly recommended!
professional carpet cleaning Phoenix 85063!
TruePills, No prescription needed, Buy pills without restrictions. Money Back Guaranteed 30-day refunds.
Trial ED Pack consists of the following ED drugs:
Viagra 100mg 5 pills
Cialis 20mg 5 pills
Levitra 20mg 5 pills
https://cutt.ly/7wC5m1Id
https://fechicheki.blogspot.com/search?q=https%3A%2F%2Ftrue-pill.top
https://bruggerfloor.ru/bitrix/redirect.php?goto=https://true-pill.top/
https://hvoost.ru/bitrix/redirect.php?event1=click_to_call&event2=&event3=&goto=https://true-pill.top/
http://www.alfakmv.ru/bitrix/redirect.php?event1=&event2=&event3=&goto=https://true-pill.top/
https://98.gregorinius.com/index/d1?diff=0&source=og&campaign=5796&content=&clickid=6glaagrcny71ype6&aurl=http%3A%2F%2Ftrue-pill.top
Extra ED Pack consists of the following ED drugs:
Viagra 100mg 20 pills
Cialis 20mg 20 pills
Levitra 20mg 20 pills
Super ED Pack consists of the following ED drugs:
Viagra 100mg 10 pills
Cialis 20mg 10 pills
Levitra 20mg 10 pills
https://cutt.ly/7wC5m1Id
https://shtory70.ru/bitrix/redirect.php?event1=click_to_call&event2=&event3=&goto=https://true-pill.top/
https://63.biqund.com/index/d1?diff=0&utm_source=ogdd&utm_campaign=26607&utm_content=&utm_clickid=sooggc0cc8o88sgk&aurl=https%3A%2F%2Ftrue-pill.top%2F&an=&utm_term=&site=&pushMode=popup
http://www.killermovies.com/out/jump.php?domain=true-pill.top
https://prigov.info/bitrix/redirect.php?goto=https://true-pill.top/
https://17.torayche.com/index/d1?diff=0&utm_source=og&utm_campaign=20924&utm_content=&utm_clickid=jok4s40c488w4ws4&aurl=http%3A%2F%2Ftrue-pill.top
Увеличим Ваши продажи в Etsy. Даю Гарантии Заказчику
Jump to search
Speculate on market Forex?
Best exclusive offer 2024 for common speculators, software developers, traders, trading signal sellers, trading advisor sellers, trading account managers, investment companies, large brokerage firms , as well as for everyone who dreams of opening their own business on the Forex market with minimal investments.
We will be happy to Give away MetaTrader4 Server for 0Give away MetaTrader4 Server for 0/en/products.html
More in detail watch here:
https://drive.google.com/file/d/14xuST2EFDKcnfUT_dL49jQu0Asj1uJx4/view?usp=sharing
50% off Sale! CyberSpace 2040’s, Creative Smartphone Wireless Charging Suspension Table Lamp, Dadypet Pet Dog Hair Dryer, Dog Leash Retractable, Dog Water Cup Drinking
Гробы для животных с эксклюзивным декором или Организация похорон через морг Москва
Правила установки памятников Хованское кладбище
https://ritualsm.ru/kresty.html
Ещё можно узнать: Организация похорон на Новом-Ямском кладбище
Эконом кресты на могилу
Manchester United’s teenage sensation Kobbie Mainoo shows the way forward in rollercoaster season
kraken18.at
No matter how successful – or lately, unsuccessful – Manchester United has been on the pitch, the club has always prided itself on an uncanny ability to generate the game’s brightest young stars. The latest breakthrough talent, it seems, is 18-year-old midfielder Kobbie Mainoo.
The teenager’s emergence from the youth academy has been one of the few bright sparks in an otherwise difficult season for the team, and the highlight of his fledgling career came during United’s thrilling 4-3 win against Wolverhampton Wanderers on Thursday.\
https://kraken26-at.com
kraken29.at
After the host had seemingly snatched a draw in the 95th minute of the match, Mainoo showed his considerable potential by scoring a winner in the dying moments.
The English youngster received the ball under pressure outside of the opposition’s box before slaloming his way towards the goal, nut-megging a Wolves defender on the way. Then, when other players might have panicked, Mainoo kept his composure and guided a perfect shot into the far corner of the net.
While his teammates celebrated wildly, Mainoo seemed to take it all in his stride as he slid towards the crowd on his knees after scoring his first Premier League goal.
https://kraken24-at.com
кракен сайт
It was a sensational moment and a goal which might change the teenager’s life forever.
Why do we have right-on-red, and is it time to get rid of it?
bs2best.at
In America, traveling through red lights on right turns has become a rule of the road. Frequently, you get honked at if you don’t speed through fast enough.
But the widespread driving practice is now coming under scrutiny, and facing government curbs, for being too dangerous.
https://bs2tsite5-cc.net
b2web2.in
Years ago, right-on-red was mostly limited to California and a few other western states. Woody Allen famously declared in “Annie Hall” that he’d never live in Los Angeles because the city’s “only cultural advantage is that you can make a right turn on a red light.”
Right-on-red spread across the country in the 1970s in response to the Arab oil embargo against the United States and oil rationing. States introduced it as a gas-savings measure: The theory was that it would reduce idling at red lights.
Congress sped up states’ adoption of right-on-red laws with a provision in the 1975 Energy Policy and Conservation Act. It tied states’ eligibility for federal energy assistance to allowing right-on-red “to the maximum extent practicable consistent with safety.”
https://bs2shops.com
спрут маркетплейс
By 1972, 13 states allowed RTOR, according to a legislative history of the practice in Connecticut. By the end of the decade, nearly every state in the country had it. (Although not New York City — and the patchwork of municipalities which do or don’t allow it only adds to the behind-the-wheel confusion.)
Investigative Journalism and Bohemia: Uncovering the Darknet
Bohemia Market Review: The Good, The Bad, and The Anonymous
Cryptocurrencies and Contraband: The Financial Backbone of Bohemia Market
Bohemia Darknet Market is one of the most famous and popular markets on the Darknet. It is secure with a wide range of products and a huge user environment. In this article, we’ll look at what makes Bohemia Darknet Market so attractive and what you need to know about it before using it.
https://darknet-link.org/Bohemiamarket.html Bohemia market
Thi cong noi that cao cap sang trong, thi cong noi that biet thu, chung cu, van phong
Pinterest for Etsy, Amazon, Ebay, Shopify, sites in 2024 year
Unique BDSM sex furniture. Black bench for whipping and pleasure. Fetish, Fetish furniture for adults. Sex furniture for punishment and pleasure. BDSM, Premium BDSM sex furniture
50% off Sale! CyberSpace 2040’s, Gravity Blanket Hand-Woven, Lazy Sofa Bean Bag Chair, New Atmosphere Smart Galaxy Star Projector, New Upgrade Portable Electric Coffee Grinder, Pet Dog Winter Clothes, Pet Nail Clippers LED
Text Inmate
https://www.contactmeasap.com/
Clip Art and Digital Image, People, Nursery Baby clipart, Holidays & Celebrations, Food & Drink, Fruits and Vegetables, Halloween, Flowers, Animals & Pets, Tattoos clipart, Skull Design, Retro & Vintage Signs, Street Art & Y2K
Ремонт квартиры или постройка дома своими руками
Источник: https://stroj-sam.ru
Увеличим Ваши продажи в Etsy https://pint77.com Даю Гарантии Заказчику
Увеличим Ваши продажи в Etsy. https://pint77.com Даю Гарантии Заказчику
Welcome to BestWedd store! Here you can find editable templates for your wedding such as wedding invitations, save the dates, video invitations, seating charts, wedding signs and more
Video. Увеличим Ваши продажи в Etsy. Даю Гарантии Заказчику
Увеличим Ваши продажи в Etsy. Pinterest + SEO+II https://pint77.com Даю Гарантии Заказчику + Artificial intelligence in action – Clip Art and Digital Image.
Wedding Invitations, Wedding Video Invitation, Short Video Itvitation, Save the Date, Wedding Backdrop, Wedding Day Slideshow
In Etsy, Amazon, eBay, Shopify – Pinterest+SEO + artificial intelligence give high sales results
In Etsy, Amazon, eBay, Shopify Pinterest+SEO + artificial intelligence give high sales results
In Etsy, Amazon, eBay, Shopify Pinterest+SEO + artificial intelligence give high sales results
[url=https://pint77.com] In Etsy, Amazon, eBay, Shopify Pinterest+SEO + artificial intelligence give high sales results[/url]
[url=https://pint77.com]How to catch big fish on pinterest[/url]
доставка вермута
Какие еще напитки мы доставляем на дом 24/7?
Source:
– http://alcomoscow07.ru/category/shampanskoe/beloe
[url=https://pint77.com]In Etsy, Shopify Pinterest+SEO + artificial intelligence give high sales results
Актуальное, рабочее зеркало официального сайта Гама https://gamacasinotoday.ru/
In Etsy, Shopify Pinterest+SEO + artificial intelligence give high sales results
In Etsy, Shopify Pinterest+SEO + artificial intelligence give high sales results
Click the link to get 100€ coupon bundle or Search acl929258 on the Temu App to get 30% off discount!
In Etsy, Amazon, eBay, Shopify https://pint77.com Pinterest+SEO +II = high sales results
In Etsy, Shopify Pinterest+SEO + artificial intelligence give high sales results
Your sales on Etsy, Amazon, ebay, shopify.
Pinterest advertising for the USA and English-speaking countries. Etsy, amazon, shopify, ebay
Pinterest advertising for the USA and English-speaking countries. Etsy, amazon, shopify, ebay
Erectile dysfunction treatments available online from TruePills.
Discreet, next day delivery and lowest price guarantee.
Viagra is a well-known, branded and common erectile dysfunction (ED) treatment for men.
It’s available through our Online TruePills service.
Trial ED Pack consists of the following ED drugs:
Viagra Active Ingredient: Sildenafil 100mg 5 pills
Cialis 20mg 5 pills
Levitra 20mg 5 pills
https://true-pill.top/
Ozvir
Robaz
Flusal
Aciherp
Pinterest advertising for the USA and English-speaking countries. Etsy, amazon, shopify, ebay
Самое интересное тут https://www.evernote.com/shard/s470/sh/ec166107-8703-6f78-e4a6-b21d99c1c8ea/OO3sBpnuYbMlSfl3fnTLQN6oWV8rx20qr0FoOBoULybcXrKdB96C3terQQ
You are sleeping – your PC is collecting crypto. The Grasse Network uses 1% of your PC to collect artificial intelligence data from the Internet. Join for free. Output in Solano